Traumatic brain injuries can contribute to both short-term and long-term issues with cognitive function, but they can also impact emotional and physical health beyond the brain itself. While much of the research to date has focused on more severe forms of traumatic brain injury, it is now expanding to evaluate concussions.
Writing this article reminded me that I, too, am part of this story. I had two episodes of concussion in my teens and early twenties, neither related to sports: one from a fall where I hit my head, another from a car accident that resulted in whiplash. In both of those cases, I was just told to rest until my head stopped hurting and then resume normal activity. Fortunately, I recovered without any long-term issues. In the decades since then, our understanding of head injuries has greatly expanded, prompting innovations in both diagnosis and treatment.
Concussions are viewed as a mild form of traumatic brain injuries and most frequently occur following an event that involves an acceleration–deceleration mechanism without actual injury to the head, such as whiplash, or the head striking an object. As we study these, researchers and clinicians are learning that these are fairly common, but often underdiagnosed.
According to the CDC, an estimated 1.6 – 3.8 million people suffer from concussions related to sports or recreational activities every year. A National Health Interview Survey in 2020 found that 6.8% of children aged 17 years and under had ever had symptoms of concussion, while only 3.9% had ever been diagnosed. [1] There is also good evidence to suggest that an athlete who has had one concussion is also more likely to suffer from multiple concussions and suffer long-term consequences. [2] Not all head injuries occur in athletes, but these are the most studied.
While the vast majority of people with concussions recover without obvious disability, people can end up with long-term cognitive, emotional and functional issues affecting quality of life – including memory issues and Alzheimer’s disease. [3] Efforts to better predict outcome from head injuries by focusing on the age, sex, type of injury and acute assessments have led to some improvement, but still fail to predict or explain the variation in healing and outcomes.
Studies in professional athletes have shown that about 80–90% are sufficiently recovered to return to playing within 7–10 days. But that means that 10-20% are not, and their recovery can take up to 3 times longer. Even taking into account variations in initial injury, this variation is difficult to explain or predict. [4]
DNA RESEARCH LINKS TO INJURY & HEALING RESPONSE
Brain injury is broken down into two phases: a primary phase and a secondary phase. The primary phase is the result of the physical or mechanical forces on the brain causing direct injury. The secondary phase involves the brain’s response to the injury – a complex interplay of multiple biological systems including immune, vascular, neuroendocrine, neurotransmitters, neuroplasticity and even mitochondria and epigenetics. [3] In concussions, it is typically this secondary phase that plays a major role in how well an individual responds and recovers – both in time and function.
DNA is the genetic code that is the blueprint for everything that goes on in our bodies. Genomics is the study of how small changes in our DNA affect how our bodies function. [See feat. on
Genomics testing] Research, primarily focused on combat veterans and athletes so far, has shown that these small variations in our DNA may account for at least some of why some people respond to and recover from traumatic brain injury better than others.
The APOE gene plays many roles, including immune response and neuroplasticity. Carriers of the APOE4 gene can be predisposed to worse outcomes after traumatic brain injuries, especially if they are moderate or severe, or there are multiple concussions. While the APOE gene is the most widely studied, there are now over a dozen others that have been identified. Variants in other genes involved in the inflammatory response, blood flow, DNA repair, neuroplasticity, learning and memory are also implicated, including TNF alpha, IL1, IL6, NOS3, ACE, COMT, NMDA receptors, BDNF, KIBRA, MAPT, PARP, MME, SLC17A7, GRIN2A. Because there are hundreds of genes impacting all of these biological systems, it is likely that there are many to be still evaluated, and outcomes are the result of the interaction of multiple genes.
As genomics contributes to our understanding of how and why individuals can vary greatly in their ability to recover from traumatic brain injuries, it is paving the way for more personalized prevention and treatment strategies for concussions. Having accessible and noninvasive technologies to provide evaluation of brain injury and ongoing recovery will be a key part of this progress.
References: (1) https://www.cdc.gov/traumaticbraininjury/concussion/index.html (2) McCrory et al. Consensus statement on concussion in sport—the 5th international conference on concussion in sport held in Berlin, October 2016. Br J Sports Med 2017;0:1–10. (3) Bennett et al. Chapter 9: Genetic Influences in Traumatic Brain Injury, in Laskowitz D, Grant G editors. Translational Research in Traumatic Brain Injury. CRC Press/Taylor and Francis Group 2016. (4) Jane McDevitt & Evgeny Krynetskiy. Genetic findings in sport-related concussions: potential for individualized medicine? Concussion 2017; 2(1)
ROBERTA KLINE, MD (Educational Dir. /Women's Diagnostic Group)
Dr. Kline is a board-certified ObGyn physician, Integrative Personalized Medicine expert, consultant, author, and educator whose mission is to change how we approach health and deliver healthcare. She helped to create the Integrative & Functional Medicine program for a family practice residency, has consulted with Sodexo to implement the first personalized nutrition menu for healthcare facilities, and serves as Education Director for several organizations including the Women’s Diagnostic Health Network, Mommies on a Mission. Learn more at
https://robertaklinemd.com/
Other recent articles by Dr. Kline:
RECOVERY TIME AND CONTINUED MONITORING OF CONCUSSION PATIENTS
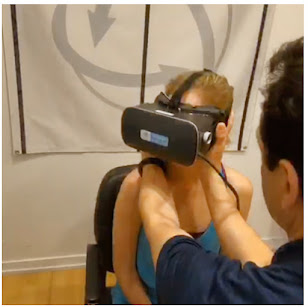
"It is imperative to constantly monitor progress of any concussion sufferer and it should be guided by current, objective testing and quantitative data", states Dr. Alex Gometz of Founder Concussion Management of New York. "You cannot rely purely only on symptoms to determine if the patient is getting better. Overall, people with a history of concussions, are more vulnerable to greater damage during future concussions. They tend to be more sensitive to lower amounts of pressure, causing similar symptoms".
In the care of concussion cases, Dr. Gometz highlights one caveat; A player with a history of a single concussion that has fully recovered (as indicated by symptoms as well as quantitative data from specific tests) can be considered to be on equal footing with players with NO history of concussion. This comparison is based on the level of vulnerability to future injuries. Studies show that full recovery from a single concussion is effective at helping players bounce back to fairly equal health as they were prior. Players with a history of concussion without full recovery do not enjoy this benefit and a future concussion can happen with less amount of force, making them more vulnerable.
Observing the common pattern in sports teams, athletes seem to return to the game sooner than non-pros. That may be due to the pressure from the organization and the player’s own drive to continue playing. This premature return contributes to setting premature standards that are clearly inadequate and potentially unrealistic. Standards need to include specific quantitative measures so that each player can demonstrate objective improvement. Schools should make sure their protocols are safe and reviewed by a medical board with proper steps and safeguards instead of copying other institutions’ protocols, following professional accountability.
CONCUSSION & PCS (Post-Concussive Symptoms)
Board Certified Chiropractic Neurologist
Imagine a 3 pound ball of jello. Now fill that ball with 86 billion tiny wires, each of which has 10,000 interconnections. Now imagine another 86 billion cells supporting those wires, all of which are surrounded by chemical messengers that help with the communication. This incredibly complex ball of jello sits inside of a sealed metal can. Now smash the can on the ground…this is a concussion.
The majority of head traumas are considered ‘mild’ or mTBI. However, there is no such thing as a mild concussion in my mind. The assessment of these injuries has been poor for decades and at this point is only slightly better than that. A neurocognitive on field evaluation or bedside exam followed by a CT scan to evaluate brain structure. The vast majority of these cases have no abnormal imaging studies, but people are left with ongoing functional neurological changes. With every concussion, there is a moment of rotation that disrupts brainstem and cervical spine function as well, but this is rarely imaged or assessed.
Up to 30% of people with mTBI have Post-Concussion Syndrome where symptoms of headache, dizziness, dysautonomia, imbalance, visual tracking problems, cognitive impairment and anxiety and depression become part of everyday life. Traditional neurologists and psychologists do their best to help patients manage symptoms, but they have no available targeted therapy to address all of the issues that these patients experience.
There are three main areas that become altered after a concussion; the brainstem, the gut and the cervical spine.
 THE BRAINSTEM
THE BRAINSTEMThis region is below the cortex and houses all of the incoming and outgoing communication from the brain to the body and back. It also contains 10 pair of cranial nerves that control eye movement, balance, facial sensation and muscle control as well as the entire parasympathetic nervous system. One of the first things that happens following a concussion is a disconnection of head-eye movement dynamics mediated by a reflex called the VOR. A thorough look at the nuances in cranial nerve testing as well as motor control and tone, saccadic eye movement (along with pursuits and vergence), VOR, balance and regulatory controls allows a trained clinician to triangulate the specific area of insult and create a neurotherapy plan to remediate it.
THE GUT
Studies have shown that within hours of a head trauma, the gut lining becomes porous and we develop a leaky gut. This leads to large diameter proteins making their way into the bloodstream, creating an altered immune state. Bacterial dysbiosis, a common imbalance in the microbiome, compounded by this increase in intestinal permeability can impair neurogenesis.
THE CERVICAL SPINE
A series of seven small vertebrae in the neck that house the upper spinal cord maintain the weight of the head. The muscular, cartilaginous and ligamentous structures in this region are central to neurological control as they are laden with sensory receptors. These muscle spindles and mechanoreceptors become altered after TBI due to a change in mechanical function of the joints holding the vertebrae together. There have been studies that show that this mechanical dysfunction alone is enough to create and recreate concussion symptoms.
Since this is now a functional neurological syndrome, a trained functional neurologist is the go to provider to help remediate the problems. A careful assessment of brainstem, gut and cervical spine function, followed by a care plan to remediate each of these areas generally leads to significant if not complete resolution of the problems.
DR. MICHAEL GRUTTADAURIA is a Board Certified Chiropractic Neurologist and Professional Biohacker. He manages a private practice in Huntington, NY, treating people with chronic health conditions from early Alzheimer's Disease, IBS, neck/back pain, anxiety/depression, dizziness, vertigo, migraines and concussion/PCS. "Dr. Mike" uses functional neurological examination and advanced testing to evaluate the body, brain and brainstem to develop strategies to rehabilitate most chronic neurological conditions. He applies interventions including functional neuro rehab, balance training, eye movement rehabilitation, chiropractic adjustments and functional nutrition. www.TheOptimumU.com
COLLECTING QUANTITATIVE DATA THROUGH SCANNING OF THE OPTIC NERVE FOR COGNITIVE DISORDERS
By: Robert L. Bard, MD
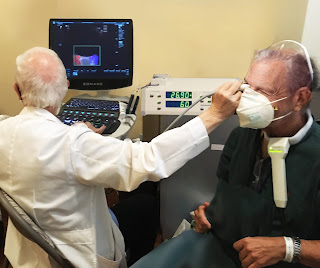
Now that radiologists are using Doppler blood flow to examine eye disease, including systemic diseases (including Diabetes, Brain tumors, heart disease, sickle cell disease etc) that affect the eye, we are hopeful that the ophthalmologic and neurological communities will start using this noninvasive technology as well to improve noninvasive and more rapid treatment of potential eye disorders, such as cancers of the eye, diabetes and glaucoma. Another future use will be to correlate the effect of decreased vascular pulsation in the production of cerebrospinal fluid that is removed by the cleansing glymphatic system is postulated as a contributing factor in degenerative neuromuscular disease.
BLOOD FLOW STUDY 101: Hemodynamics is defined as the study of blood flow in relation to the status of the circulatory system and homeostatic mechanisms of autoregulation. Through the monitoring of blood flow, diagnostic analysis can provide many answers to the health and physiological status of the target area scanned as well as cell-level metabolism, the regulation of the pH, osmotic pressure and temperature of the whole body, and the protection from microbial and mechanical harm. Assessing injuries, inflammation or mutative growths (like cancer tumors), assessment of blood flow provides diagnostic answers about the severity of tissue disorders or tumor malignancy.** ALSO SEE DR. BARD'S ULTRASONIC REVIEW ON CONCUSSION AND COGNITIVE ASSESSMENT

July 19, 2022- IPHA NEWS conducted a private interview with the co-developers of NEUROVINE - a portable headband using EEG (electroencephalogram) technology to measure brain waves. Meet CEO Ashleigh Kennedy, Ph.D., and CMO Matthew Kennedy, MD, MSc (co-founders of Neurovine) from Ottawa, Ontario, CA. who shares their objectives in support of concussion monitoring by measuring brain health as part of optimizing their recovery processNeurovine offers this portable interactive monitoring program for athletes, students, professionals and anyone undergoing mentally strenuous work by “alerting them to take brain breaks before an activity becomes too strenuous”.
PAIN 101: THE MIND-BODY CONNECTION By: Josh T. Schueller
Pain is everywhere. Billions of dollars are spent each year in the United States alone on pain treatments and remedies. Per the National Center for Health Statistics almost 60% are living with pain. While most sufferers of pain want relief and answers, many medical professionals may be providing inefficient or incorrect pain reliefs counters. The “cookie cutter” approach for pain over the last several decades has left the world in a pain crisis. One of the main reasons why- the current treatment model does not do an adequate job in categorizing pain. Pain falls under different categories. Most people do not understand that the type of pain you have directly correlates the type of treatment given. Personalized medicine in the treatment of pain holds the key to understanding the types of pain and developing the correct course of action to treat the pain.
Disclaimer: MEDTECH REVIEWS* is a non-commercial user review of health-related technologies and is not intended as a marketing program for any device(s) featured in this video for evaluation. This presentation is for informational use only does not offer any direct medical claims whatsoever. Statements from all speakers herein are expressing their own unscripted views that do not reflect those of our producers. Always seek the advice of your physician or other qualified health care provider with any questions you may have regarding a medical condition or treatment.
Copyright Notice: The materials provided on this website/web-based article are copyrighted and the intellectual property of the publishers/producers (The NY Cancer Resource Alliance/IntermediaWorx inc. and The AngioFoundation). It is provided publicly strictly for informational purposes within non-commercial use and not for purposes of resale, distribution, public display or performance. Unless otherwise indicated on this web based page, sharing, re-posting, re-publishing of this work is strictly prohibited without due permission from the publishers. Also, certain content may be licensed from third-parties. The licenses for some of this Content may contain additional terms. When such Content licenses contain additional terms, we will make these terms available to you on those pages (which his incorporated herein by reference).The publishers/producers of this site and its contents such as videos, graphics, text, and other materials published are not intended to be a substitute for professional medical advice, diagnosis, or treatment. For any questions you may have regarding a medical condition, please always seek the advice of your physician or a qualified health provider. Do not postpone or disregard any professional medical advice over something you may have seen or read on this website. If you think you may have a medical emergency, call your doctor or 9-1-1 immediately. This website does not support, endorse or recommend any specific products, tests, physicians, procedures, treatment opinions or other information that may be mentioned on this site. Referencing any content or information seen or published in this website or shared by other visitors of this website is solely at your own risk. The publishers/producers of this Internet web site reserves the right, at its sole discretion, to modify, disable access to, or discontinue, temporarily or permanently, all or any part of this Internet web site or any information contained thereon without liability or notice to you.
 "It is imperative to constantly monitor progress of any concussion sufferer and it should be guided by current, objective testing and quantitative data", states Dr. Alex Gometz of Founder Concussion Management of New York. "You cannot rely purely only on symptoms to determine if the patient is getting better. Overall, people with a history of concussions, are more vulnerable to greater damage during future concussions. They tend to be more sensitive to lower amounts of pressure, causing similar symptoms".
"It is imperative to constantly monitor progress of any concussion sufferer and it should be guided by current, objective testing and quantitative data", states Dr. Alex Gometz of Founder Concussion Management of New York. "You cannot rely purely only on symptoms to determine if the patient is getting better. Overall, people with a history of concussions, are more vulnerable to greater damage during future concussions. They tend to be more sensitive to lower amounts of pressure, causing similar symptoms". 










.jpg)





