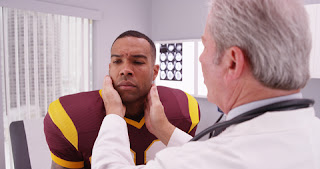
Writing this article reminded me that I, too, am part of this story. I had two episodes of concussion in my teens and early twenties, neither related to sports: one from a fall where I hit my head, another from a car accident that resulted in whiplash. In both of those cases, I was just told to rest until my head stopped hurting and then resume normal activity. Fortunately, I recovered without any long-term issues. In the decades since then, our understanding of head injuries has greatly expanded, prompting innovations in both diagnosis and treatment.
According to the CDC, an estimated 1.6 – 3.8 million people suffer from concussions related to sports or recreational activities every year. A National Health Interview Survey in 2020 found that 6.8% of children aged 17 years and under had ever had symptoms of concussion, while only 3.9% had ever been diagnosed. [1] There is also good evidence to suggest that an athlete who has had one concussion is also more likely to suffer from multiple concussions and suffer long-term consequences. [2] Not all head injuries occur in athletes, but these are the most studied.
Studies in professional athletes have shown that about 80–90% are sufficiently recovered to return to playing within 7–10 days. But that means that 10-20% are not, and their recovery can take up to 3 times longer. Even taking into account variations in initial injury, this variation is difficult to explain or predict. [4]
DNA RESEARCH LINKS TO INJURY & HEALING RESPONSE
The APOE gene plays many roles, including immune response and neuroplasticity. Carriers of the APOE4 gene can be predisposed to worse outcomes after traumatic brain injuries, especially if they are moderate or severe, or there are multiple concussions. While the APOE gene is the most widely studied, there are now over a dozen others that have been identified. Variants in other genes involved in the inflammatory response, blood flow, DNA repair, neuroplasticity, learning and memory are also implicated, including TNF alpha, IL1, IL6, NOS3, ACE, COMT, NMDA receptors, BDNF, KIBRA, MAPT, PARP, MME, SLC17A7, GRIN2A. Because there are hundreds of genes impacting all of these biological systems, it is likely that there are many to be still evaluated, and outcomes are the result of the interaction of multiple genes.
As genomics contributes to our understanding of how and why individuals can vary greatly in their ability to recover from traumatic brain injuries, it is paving the way for more personalized prevention and treatment strategies for concussions. Having accessible and noninvasive technologies to provide evaluation of brain injury and ongoing recovery will be a key part of this progress.
References: (1) https://www.cdc.gov/traumaticbraininjury/concussion/index.html (2) McCrory et al. Consensus statement on concussion in sport—the 5th international conference on concussion in sport held in Berlin, October 2016. Br J Sports Med 2017;0:1–10. (3) Bennett et al. Chapter 9: Genetic Influences in Traumatic Brain Injury, in Laskowitz D, Grant G editors. Translational Research in Traumatic Brain Injury. CRC Press/Taylor and Francis Group 2016. (4) Jane McDevitt & Evgeny Krynetskiy. Genetic findings in sport-related concussions: potential for individualized medicine? Concussion 2017; 2(1)
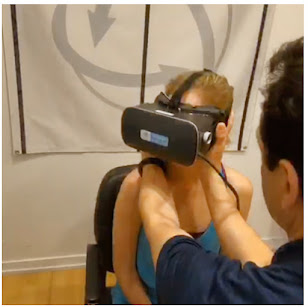 "It is imperative to constantly monitor progress of any concussion sufferer and it should be guided by current, objective testing and quantitative data", states Dr. Alex Gometz of Founder Concussion Management of New York. "You cannot rely purely only on symptoms to determine if the patient is getting better. Overall, people with a history of concussions, are more vulnerable to greater damage during future concussions. They tend to be more sensitive to lower amounts of pressure, causing similar symptoms".
"It is imperative to constantly monitor progress of any concussion sufferer and it should be guided by current, objective testing and quantitative data", states Dr. Alex Gometz of Founder Concussion Management of New York. "You cannot rely purely only on symptoms to determine if the patient is getting better. Overall, people with a history of concussions, are more vulnerable to greater damage during future concussions. They tend to be more sensitive to lower amounts of pressure, causing similar symptoms". COLLECTING QUANTITATIVE DATA THROUGH SCANNING OF THE OPTIC NERVE FOR COGNITIVE DISORDERS
By: Robert L. Bard, MD
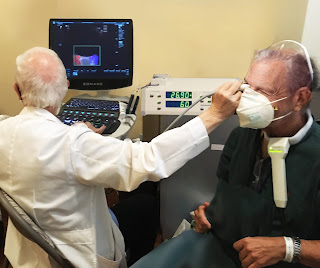
Case studies with a presumptive degenerative neuromuscular disease or amyotrophic lateral sclerosis are now being examined through a non-invasive investigation of the eye. We can observe increased intracranial pressure, which may reflect in changes in the optic nerve diameter. [Fig. 1] Scanning the eye (L) with a Doppler ultrasound probe shows the optic nerve diameter of five millimeters ®. And the right is almost eight millimeters. So we have a guide as to where the brain disease is more severe. At this point, we activate the blood flow function and look at the right eye and see that the blood flow from the anterior cerebral artery circulation that supplies the back of the eye is approximately 60 per second in the blood flow which corresponds to the graph on the bottom. [Fig. 2] On the left eye. The same blood vessel shows a decreased pressure of approximately 45 as shown by the decreased height of the blood flow graph at the bottom. Once again, we have measurable diagnostic technologies that are noninvasive, so we can follow treatment in diseases that are affecting the eye and as it relates to brain and degenerative neuromuscular disorders.Now that radiologists are using Doppler blood flow to examine eye disease, including systemic diseases (including Diabetes, Brain tumors, heart disease, sickle cell disease etc) that affect the eye, we are hopeful that the ophthalmologic and neurological communities will start using this noninvasive technology as well to improve noninvasive and more rapid treatment of potential eye disorders, such as cancers of the eye, diabetes and glaucoma. Another future use will be to correlate the effect of decreased vascular pulsation in the production of cerebrospinal fluid that is removed by the cleansing glymphatic system is postulated as a contributing factor in degenerative neuromuscular disease.
BLOOD FLOW STUDY 101: Hemodynamics is defined as the study of blood flow in relation to the status of the circulatory system and homeostatic mechanisms of autoregulation. Through the monitoring of blood flow, diagnostic analysis can provide many answers to the health and physiological status of the target area scanned as well as cell-level metabolism, the regulation of the pH, osmotic pressure and temperature of the whole body, and the protection from microbial and mechanical harm. Assessing injuries, inflammation or mutative growths (like cancer tumors), assessment of blood flow provides diagnostic answers about the severity of tissue disorders or tumor malignancy.
** ALSO SEE DR. BARD'S ULTRASONIC REVIEW ON CONCUSSION AND COGNITIVE ASSESSMENT
Pain is everywhere. Billions of dollars are spent each year in the United States alone on pain treatments and remedies. Per the National Center for Health Statistics almost 60% are living with pain. While most sufferers of pain want relief and answers, many medical professionals may be providing inefficient or incorrect pain reliefs counters. The “cookie cutter” approach for pain over the last several decades has left the world in a pain crisis. One of the main reasons why- the current treatment model does not do an adequate job in categorizing pain. Pain falls under different categories. Most people do not understand that the type of pain you have directly correlates the type of treatment given. Personalized medicine in the treatment of pain holds the key to understanding the types of pain and developing the correct course of action to treat the pain.








.jpg)